Australian Asthma Handbook
The National Guidelines for Health Professionals
Directory of guidance on managing asthma in each age group.

Adults and Adolescents
The basics of asthma care for people 12 years and over.

Principles of management
Goals and principles of asthma management in adults and adolescents.
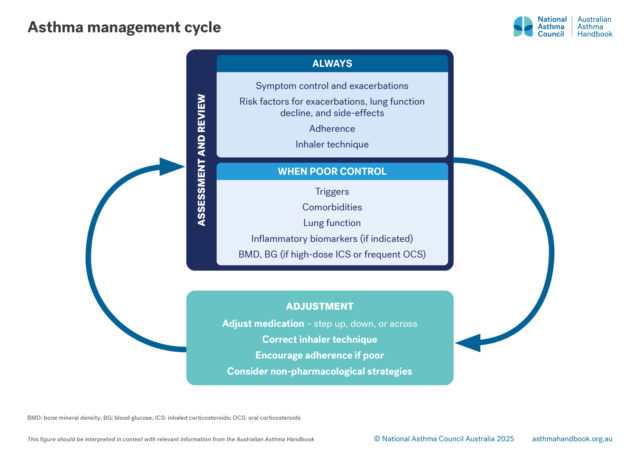
Principles of management
How to assess asthma control and severity. Risk factors for asthma exacerbations and what to include at check-ups for…

Principles of management
How to choose and use asthma inhalers for adults and adolescents.

Principles of management
How to equip and coach patients to manage their own asthma, including exacerbations.
Adults and Adolescents
Prescribing asthma treatment for people 12 years and over.

Medication management
How to choose optimal starting treatment for patients 12 years and over.
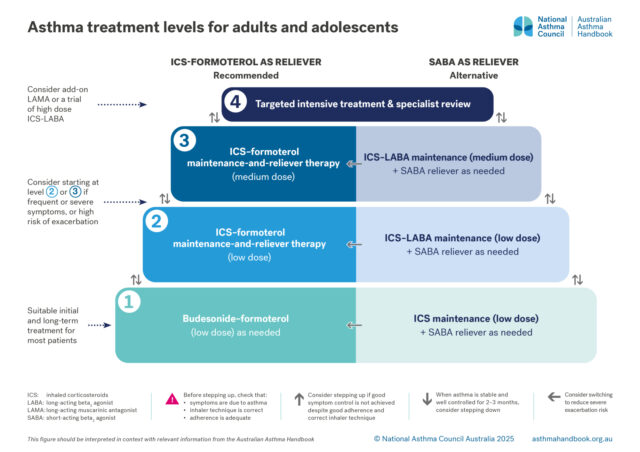
Medication management
Recommended and alternative treatment options for patients 12 years and over, according to intensity of treatment…

Medication management
How to step up or step down asthma treatment for an individual patient to maintain control and minimise side-effects.

Medication management
How to investigate asthma that is not well controlled despite treatment with medium-dose ICS-LABA

Medication management
Overview of specialist management of severe asthma in patients 12 years and over. Practical advice for primary care…

Adults and Adolescents
Trigger avoidance, allergen immunotherapy, and holistic asthma care for people 12 years and over.

Adjunctive management
What to advise patients about avoiding exposures that trigger their asthma.

Adjunctive management
When to consider allergen immunotherapy for patients with allergic asthma.

Adjunctive management
Advising patients on diet, exercise, healthy weight, and breathing exercises

Children 6-11 years
The basics of asthma care for primary school children for primary school children.

Principles of management
Goals and principles of asthma management in primary school-aged children.

Principles of management
How to assess asthma control and severity in children. Risk factors for asthma exacerbations and what to includes at…

Principles of management
How to administer inhaled medicines to children.

Principles of management
How to equip and coach children and their parents to manage childhood asthma, including exacerbations.

Children 6-11 years
Prescribing asthma treatment for primary school children.

Medication management
How to choose optimal starting treatment for children aged 6–11 years.
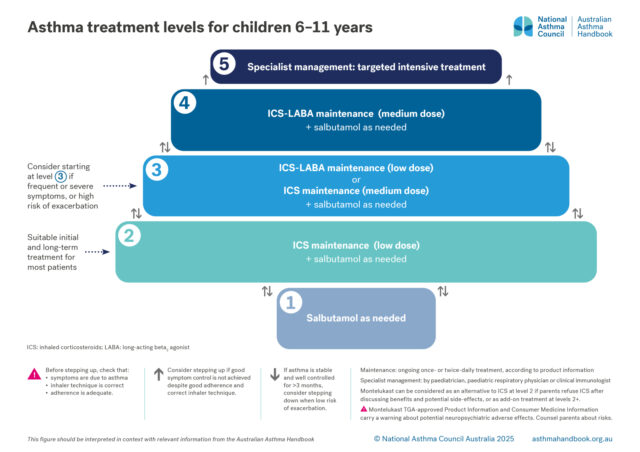
Medication management
Treatment options for primary school-aged children, classified according to the intensity of treatment needed to…

Medication management
How to step up or step down asthma treatment for a child aged 6–11 years, to maintain symptom control, prevent…
Medication management
How to manage a child’s mild asthma exacerbations that do not require an ED visit.

Medication management
How to investigate asthma that is not well controlled despite treatment with medium-dose ICS-LABA.

Medication management
Overview of specialist management of severe asthma in patients aged 6–11 years. Practical advice for primary care…

Children 6-11 years
Trigger avoidance, allergen immunotherapy, and holistic asthma care for primary school children.

Adjunctive management
What to advise parents about avoiding exposures that trigger their child’s asthma.

Adjunctive management
When to consider allergen immunotherapy for children 6–11 years with allergic asthma.

Adjunctive management
Advising parents about exercise and diet.

Children 1-5 years
The basics of asthma care for preschool children.

Principles of management
Goals and principles of asthma management in preschool children.

Principles of management
How to assess asthma control and severity in preschool children. Risk factors for asthma exacerbations and what to…

Principles of management
How to administer inhaled medicines to preschool children.

Principles of management
How to equip and coach parents and carers to manage a preschool child’s asthma, including exacerbations.

Children 1-5 years
Prescribing asthma treatment for preschool children.

Medication management
How to choose optimal starting treatment for preschool children.
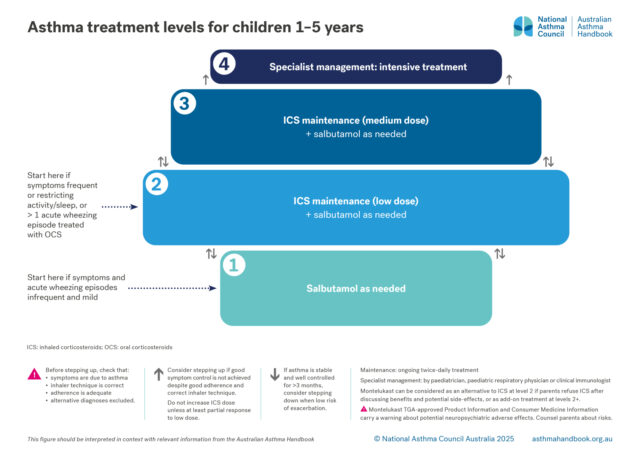
Medication management
Treatment options for preschool children, classified according to intensity of treatment needed to control asthma…

Medication management
How to adjust asthma treatment for a preschool child to maintain symptom control, prevent acute exacerbations, and…
Medication management
How to manage a preschool child’s mild asthma exacerbations that do not require an ED visit.

Children 1-5 years
Trigger avoidance and holistic asthma care for preschool children.

Adjunctive management
What to advise parents about avoiding exposures that trigger their child’s asthma.

Adjunctive management
Advising parents about exercise and diet.